How Gluten Intolerance Causes Weak Bones
Did you know that 75% of all celiac disease patients have low bone density (osteopenia) and that nearly 40% of all celiac disease patients have full-blown osteoporosis?
Osteoporosis is the quintessential silent disease. Most people only learn they suffer from the disease after they break a bone. This lesson will help you identify this stealthy pest and treat it before it is too late. It will also illuminate the surprising ways gluten antibodies affect bone formation. The celiac disease and osteoporosis connection is more strong and multifaceted than many people realize.
One important part of this lesson discusses how newly diagnosed celiac patients need to be careful about taking prescription resorption agents. If a doctor treats your osteoporosis with these important medications before identifying the presence of celiac disease, the consequences can be severe.
- What Is Osteoporosis?
- Osteoporosis And Celiac Disease
- IMPORTANT: New Celiacs, Beware of Bone Resorption Agents
- How Gluten Antibodies Attack Your Bones
- Osteoporosis Symptoms
- Calcium Deficiency Symptoms
- Magnesium Deficiency Symptoms
- Vitamin D Deficiency Symptoms
- Osteoporosis Risk Factors
- Diet For Bone Health
- Exercise For Bone Health
- Inflammation And Bone Mass
- Gluten And Osteoporosis
- Nutritional Suggestions
What Is Osteoporosis?
Osteoporosis is a condition where bones have become brittle, porous and weak. The term itself literally means “porous bones.” Bone tissue requires constant renewing through a process called bone remodeling. As older bone tissue is absorbed into the bloodstream as minerals, a process called resorption, new bone tissue must be made through a process called formation.
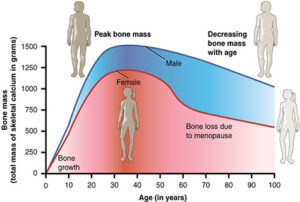
Osteoporosis occurs when resorption greatly exceeds formation for an extended period of time. Between the ages of 30 and 40, most adults reach a point where bone resorption begins to exceed bone formation. Exercise and diet must be adjusted to compensate for this inevitable consequence of aging.
Osteoporosis is a serious and widespread medical problem. Current estimates suggest osteoporosis costs $18 billion each year in the United States medical system.
Recent research suggests about ten million people in the United States alone suffer from osteoporosis, and about eighteen million more Americans suffer from low bone mass (osteopenia). Around 55% of all adults aged 50 and over suffer from osteoporosis.
The consequences of osteoporosis include breathing problems from poor skeletal integrity, chronic back and hip pain, reduced height, stooped posture, and most dangerously, a greatly increased risk for bone fracture. Even relatively minor events, such as coughing, can cause fractures in long-time osteoporosis patients.
Osteoporosis And Celiac Disease
Osteoporosis is pervasive in the modern world, and it is even more pervasive in patients of celiac disease. It is one of the most common consequences of celiac disease. About 75 percent of newly diagnosed celiac patients suffer from low bone mass, and nearly 40% of adult celiac patients have full-blown osteoporosis.
Osteoporosis is one of the silent symptoms of celiac disease. There are no tangible outward symptoms. Osteoporosis often isn’t discovered until the patient experiences a fracture from a fall or accident. By then, the damage is done and restoring healthy bone mass can be a great challenge.
Celiac disease exerts its earliest and most severe damage to the duodenum in the proximal small intestine, the part of the small intestine best able to absorb critical bone nutrients like calcium, magnesium and vitamin D.
Everyone diagnosed with celiac disease should have their bone mass screened, and every adult diagnosed with celiac disease should monitor their intake of calcium, magnesium and vitamin D, even before their bone mass is measured.
Discuss all supplements with your doctor. While magnesium and vitamin D appear to be safe in most cases, some evidence suggests calcium supplements may increase cardiovascular episodes in at-risk individuals.
New Celiacs: Beware of Bone Resorption Agents
While prescription bone resorption agents are necessary for people trying to recover from serious cases of osteoporosis — where a combination of supplements and exercise don’t appear to be enough — these resorption agents can be problematic for newly diagnosed celiac disease patients.
It is important for celiac disease patients to use a gluten-free diet and good health habits to repair their small intestine before taking resorption agents. This is because resorption agents block your body from taking minerals from your bone and adding them to your blood. When organs need calcium or magnesium, the hormone PTH signals the bones to add these minerals to the bloodstream. Resorption agents stop this natural process.
If your small intestine has been significantly damaged by celiac disease, you probably don’t properly absorb minerals from your diet. Thus, the combination of a damaged small intestine and resorption agents can lead to severely low blood levels of important minerals like calcium and magnesium, which play an integral role in the health and regulation of muscles, nerves and your heart.
So if you have been concerned about gluten intolerance symptoms and your doctor prescribes resorption agents, you should be tested for celiac disease first. If you are diagnosed with celiac disease, you need to go on a strict gluten-free diet and heal your gut before you begin taking the resorption agents.
Disclaimer: As always, you should take your doctor’s specific advice for you over any advice you read online. Please don’t stop taking prescribed resorption agents without talking to your doctor if you have self-diagnosed yourself as gluten intolerant.
How Gluten Antibodies Attack Your Bones
Tissue transglutaminase (tTG) — an enzyme that acts on the gluten protein gliadin in the small intestine of celiac disease patients — also performs normal functions in other places throughout the body, including in the skin and bones.
While the research is still preliminary in this area, at this point reputable researchers believe antibodies to tTG may block the function of tTG in the bones of celiac disease patients, which results in suppressed bone formation.
For this reason, gliadin consumption, which in celiac patients causes antibodies to tTG, may contribute to an autoimmune response in the bones. This prevents them from replenishing bone mass lost through resorption. This may illuminate why osteoporosis is common even in celiac disease patients with normal and healthy calcium and vitamin D levels.
While gluten doesn’t appear to have as significant an impact on bone health for people without any form of gluten intolerance, a diet high in wheat products, especially products made from refined wheat flour, may result in a diet high in carbohydrates. High glycemic diets contribute to elevated insulin and cortisol levels. High insulin and cortisol can leach minerals from your bones.
Osteoporosis Symptoms
Even independent of celiac disease, osteoporosis is often referred to as a silent disease. Most people with osteoporosis won’t realize they have the condition until they break a bone.
In relatively healthy people under 40, outward symptoms often don’t occur at all. However, in severe cases or in older adults, the following symptoms may occur:
- Back pain
- Easy bone fracture from a minor event, where the fracture is unexpected from the event
- Frequent bone fractures
- Hip pain
- Kyphosis, or a hump-like spine curvature
- Loss of height
- Stooped posture
In addition, I recommend monitoring for the following symptoms of calcium, magnesium or vitamin D deficiencies.
Symptoms of Calcium Deficiency
- Anxiety or feeling jittery
- Brittle nails
- Heart palpitations
- Insomnia
- Irritability
- Muscle cramps
- Muscle spasms
- Poor blood clotting
- Tooth decay or poor dental health in general
Symptoms of Magnesium Deficiency
- Abnormal heart rhythms
- Fatigue
- Loss of appetite
- Muscle spasms and cramps
- Nausea
- Numbness
- Personality changes
- Tingling in extremities
Symptoms of Vitamin D Deficiency
- Burning sensation in your mouth
- Diarrhea
- Excessive scalp perspiration
- Insomnia
- Myopia (nearsightedness)
- Nervousness
Note that the most common cause of childhood rickets is a vitamin D deficiency. If your doctor diagnoses your child with rickets, you might want to make sure celiac disease isn’t the origin.
Osteoporosis Risk Factors
In addition to celiac disease, the following factors will increase your risk for osteoporosis:
- Age – the older you are, the greater your risk
- Alcoholism
- Anorexia nervosa
- Being female, especially a postmenopausal woman
- Chronic inflammation
- Chronic stress
- Excess caffeine consumption
- Heredity
- High glycemic diet (a diet high in sugars and/or refined grains)
- Long-term use of corticosteroids, diuretics and thyroid medications
- Low estrogen (including after menopause)
- Poor diet (see below for detail)
- Rheumatoid arthritis
- Sedentary lifestyle
- Smoking
- Thyroid disease
While osteoporosis is more common in women than men, it often is more severe when it occurs in men. At about age 75 and older, the risk is about the same for men and women.
Diet For Bone Health
Diet can have a huge impact on your risk for osteoporosis. If your diet is high in sodium, you increase your risk. If your diet or lifestyle is low in one or more of the following nutrients, you significantly increase your risk: calcium, magnesium, vitamin D, vitamin K.
If you have a high sugar or high-glycemic diet, you might reduce bone mass through a process that results in high insulin and high cortisol in your blood. High insulin triggers secretion of the stress hormone cortisol. Insulin and cortisol together leach calcium from your bones and bring it into the bloodstream. If enough calcium is leached into your bloodstream, your kidneys will filter it out of your blood and into your urine for elimination.
Exercise For Bone Health
A sedentary lifestyle can also increase your risk or exacerbate your condition. You need regular exercise, particularly resistance training or weight-bearing exercise, to maintain strong bones.
Dozens of studies support how weight-bearing or resistance-bearing exercise helps not only maintain healthy bone density, but improve it. In older women, in particular, several studies showed that doing high intensity resistance training just twice a week for a year could increase bone density and greatly improve overall musculoskeletal health. Specifically, you should try to target closed-chain kinetic exercises. That is, resistance with a fixed surface, for example, squats and lunges for the lower body and push-ups and pull-ups for the upper body.
I recommend working with your doctor or a professional trainer. Let them guide you on the safest, most effective exercise routine for your anatomy and fitness level.
Inflammation And Bone Mass
When you experience significant inflammation, your body produces inflammatory mediators called cytokines. These cytokines course through your blood and affect tissues throughout your body, often causing new and different inflammatory problems. If you experience chronic inflammation, these cytokines, along with other inflammatory mediators, may attack bone tissue and suppress appropriate bone formation.
Inflammation can also trigger cortisol secretion, and as I mentioned earlier, high cortisol levels can leach calcium from your bones.
Gluten And Osteoporosis
Both celiac disease and a non-celiac gluten sensitivity (NCGS) cause inflammation of the small intestine and gastrointestinal distress, though it is far more severe and well-established with celiac disease. This can reduce your ability to absorb critical bone nutrients like calcium, magnesium and vitamin D.
Both conditions also cause systemic inflammation, causing pro-inflammatory cytokines and cortisol to course through your veins, potentially suppressing bone development and leaching calcium from your bones.
In people with some forms of gluten intolerance (most likely celiac disease, dermatitis herpetiformis and gluten ataxia), gluten triggers an autoimmune response to the antibody tTG, which performs necessary functions in the bones. This autoimmune response may suppress bone formation.
There doesn’t appear to be a direct impact of gluten consumption on bone density in people who don’t have some kind of clinically diagnosed form of gluten intolerance. However, a diet high in wheat products may be excessively high in simple carbohydrates. A high glycemic diet can result in elevated insulin and cortisol levels, which can result in calcium being leached into your bloodstream. If calcium levels in your blood become too high, your kidneys will filter this critical mineral out of your blood and into your urine for elimination instead of allowing it to re-enter your bones from your blood.
Nutritional Suggestions
The most important nutrients to target are calcium, magnesium, vitamin D and vitamin K.
Calcium, magnesium and vitamin K can be obtained through a good diet, but depending on your profession, lifestyle, and where you live, you may need to take a vitamin D supplement. This is because your body makes vitamin D when you expose your skin to plenty of sunshine without wearing sunscreen. Because of modern lifestyles and the concern for skin cancer, people rarely obtain the regular sun exposure they need to maintain healthy vitamin D levels.
There are two forms of vitamin D available as supplements, vitamin D2 (ergocalciferol) and vitamin D3 (cholecalciferol). Vitamin D3 is the type your body makes when skin is exposed to sun, and evidence suggests it might be slightly safer while it also raises vitamin D levels faster than vitamin D2. In the past, vitamin D3 was only available sourced from fish oil or sheep lanolin, but recent developments allow vegans to obtain the benefits of D3 sourced from lichen, a kind of algae that grows on the surfaces of sunlit rocks.
Try to avoid foods that may inhibit absorption of these nutrients at the same time you eat foods rich in these nutrients. For example, it isn’t a good idea to eat a large portion of unfermented soy product at the same time you consume your primary source of calcium. The phytic acid in unfermented soy binds to some of the calcium and prevents your body from absorbing it. Drinking larger quantities of popular soft drinks (soda pop) may also have the same effects as these drinks are high in phosphorus.
Foods rich in vitamin C can help counteract the effects of phytic acid, and some enzyme supplements include phytase, an enzyme that counteracts phytic acid. So if you often consume your source of calcium with legumes or grains, try to eat something rich in vitamin C or take a phytase supplement at the same time.
Remember to aim for a low-glycemic diet. Moderate carbohydrate intake, and when you do consume carbohydrates, they should come in the form of whole, complex foods rather than added sugars or refined grains.
Don’t Forget, Excuse or Procrastinate Exercise
Exercise — resistance training in particular — is critical in the overall picture of building and maintaining healthy bones. Don’t make the common mistake of thinking or hoping a special diet or special supplements will allow you to avoid exercise.
Categories: Autoimmune Diseases, Celiac Disease, Non-Celiac Gluten Sensitivity